Employer-sponsored healthcare costs are climbing sharply in 2026, adding pressure to corporate margins already strained by higher labor and operating expenses.
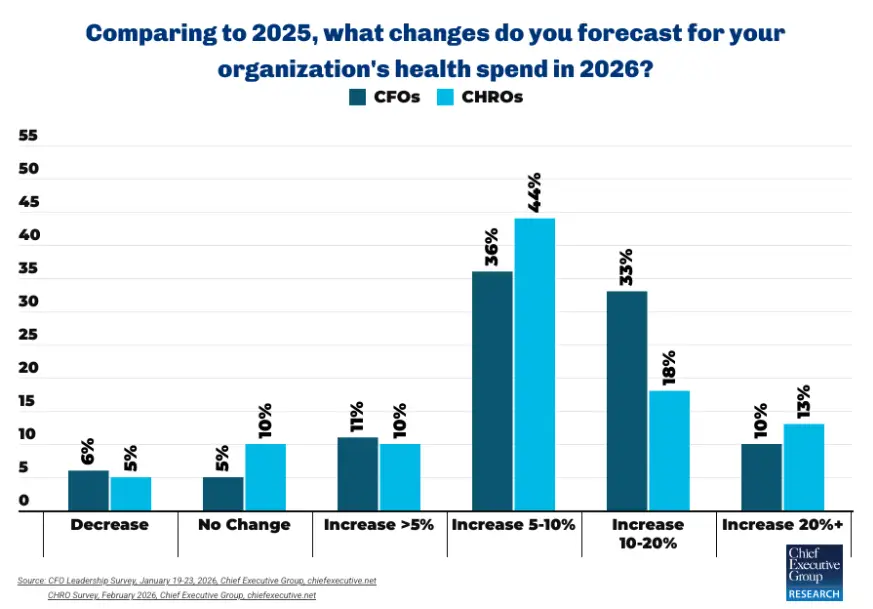
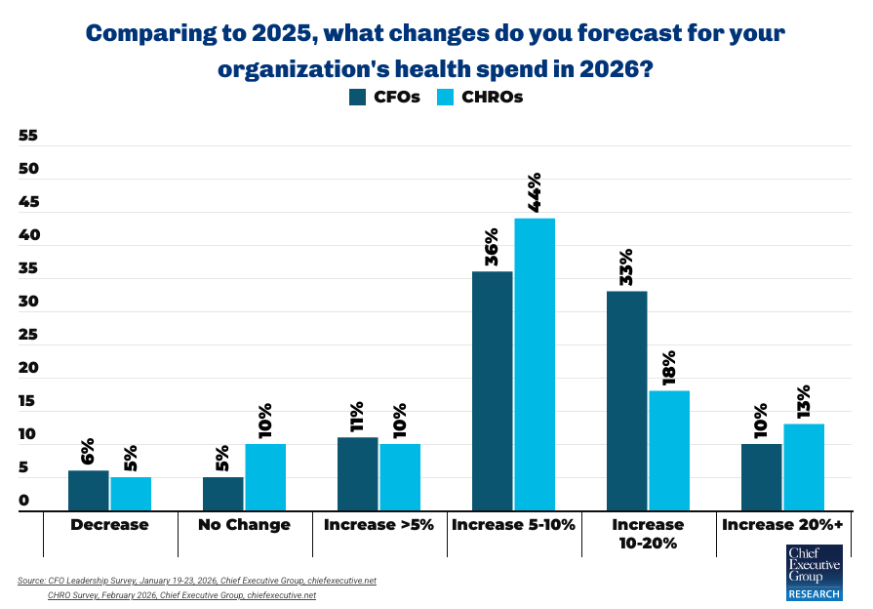
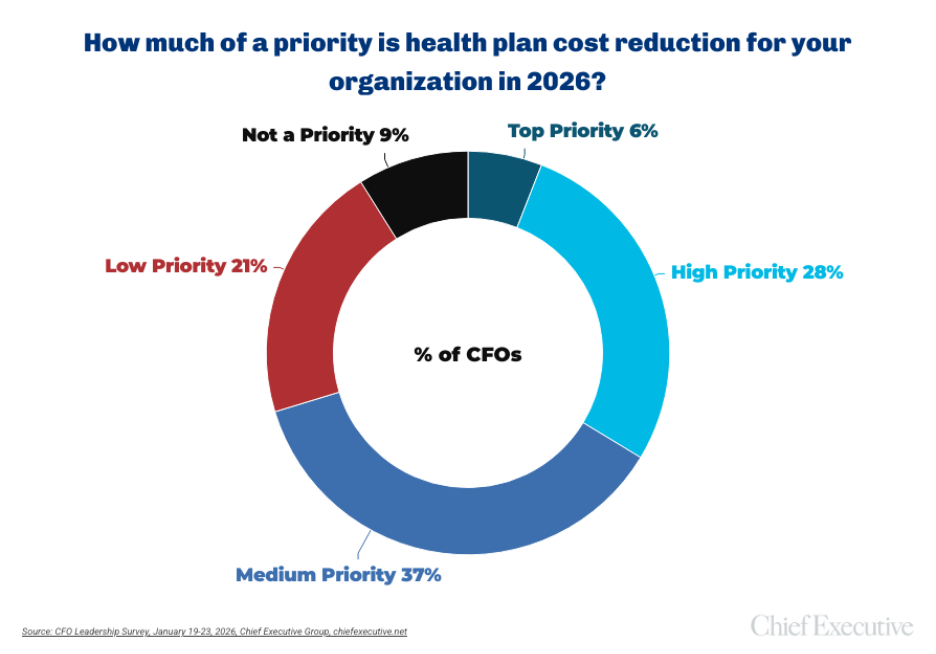
Yet only 6 percent of CFOs surveyed by CFO Leadership in January say reducing healthcare spend is a top priority for their organization, despite the fact that nine in 10 report rising premiums—and 43 percent expect those increases to be in the double digits.
CHROs report similar pressures: 85 percent say healthcare costs per employee are up in 2026, and roughly one-third cite increases exceeding 10 percent.
The outlook is consistent with sentiment among chief executives: 81 percent told sister publication Chief Executive in February their healthcare costs are increasing this year, with 43 percent projecting rises above 10 percent.
Healthcare remains one of the largest operating cost categories for U.S. employers. According to Aon’s 2025 survey data, employers subsidize roughly 80 percent of total premium costs for employer-sponsored plans, with employees covering the remainder.
“Year over year premium increases of 20 percent are unsustainable,” said one HR chief, echoing others.
Yet the survey suggests many companies feel constrained in their ability to act.
Only 14 percent of CFOs consider themselves “very informed” about alternatives to the traditional healthcare model. At the same time, 95 percent say they trust their broker or advisor to provide complete and unbiased information—over any other source—and 70 percent say they are confident their broker communicates all of the healthcare models and strategies available to their organization.
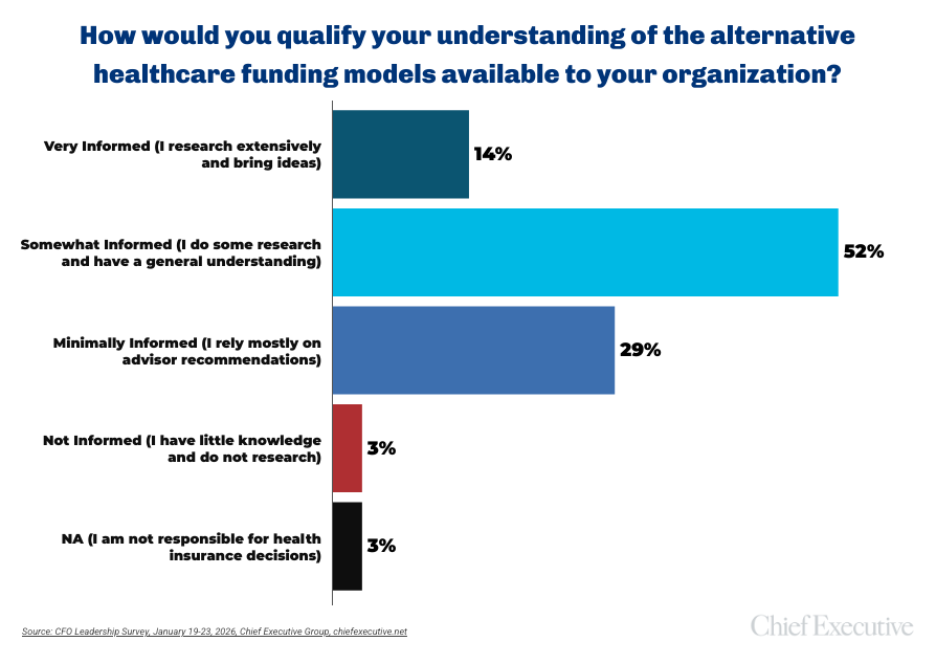
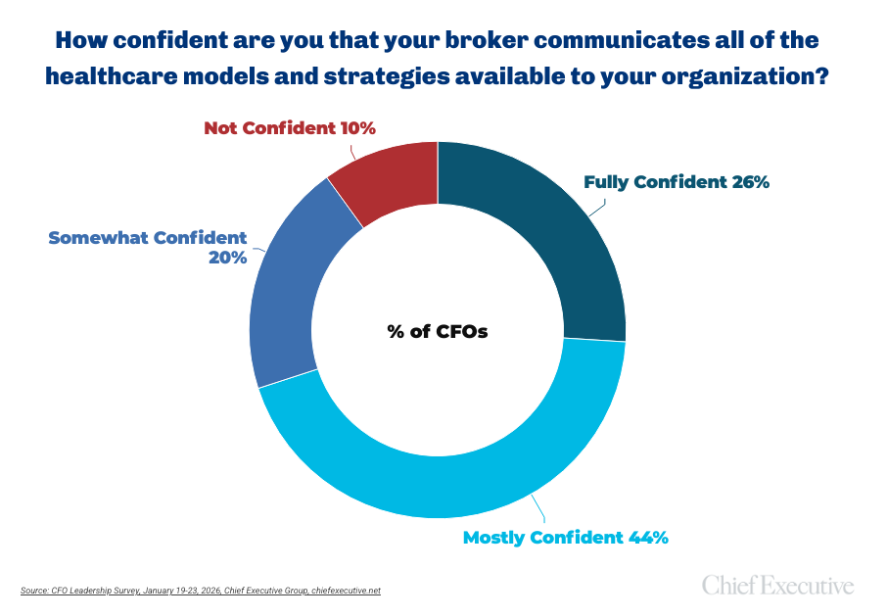
Some executives describe the issue less as indifference and more as limited leverage. “Cost increases by carriers sometimes come as a surprise, with little transparency or flexibility,” as one CFO explains. “To avoid changing carriers and causing disruption for our employees, sometimes we have to just deal with what the carriers demand.”
Michael A. Schroeder, founder and president of Roundstone Insurance, says employers often narrow their options by waiting too long to evaluate their plans. “Employers have to get off this idea that it’s a 12-month cycle that they look at with two months to go in the calendar year or the fiscal year,” Schroeder says. “That approach is going to put them in a bad place where they find out in November they’re getting a 20 percent increase.”
Instead, he says, leadership teams that begin evaluating options earlier in the year may have greater flexibility when renewal season arrives.
Paying More, Receiving the Same
Adding to the pressure is the fact that rising premiums have not consistently translated into richer benefits.
Among the CHROs we surveyed:
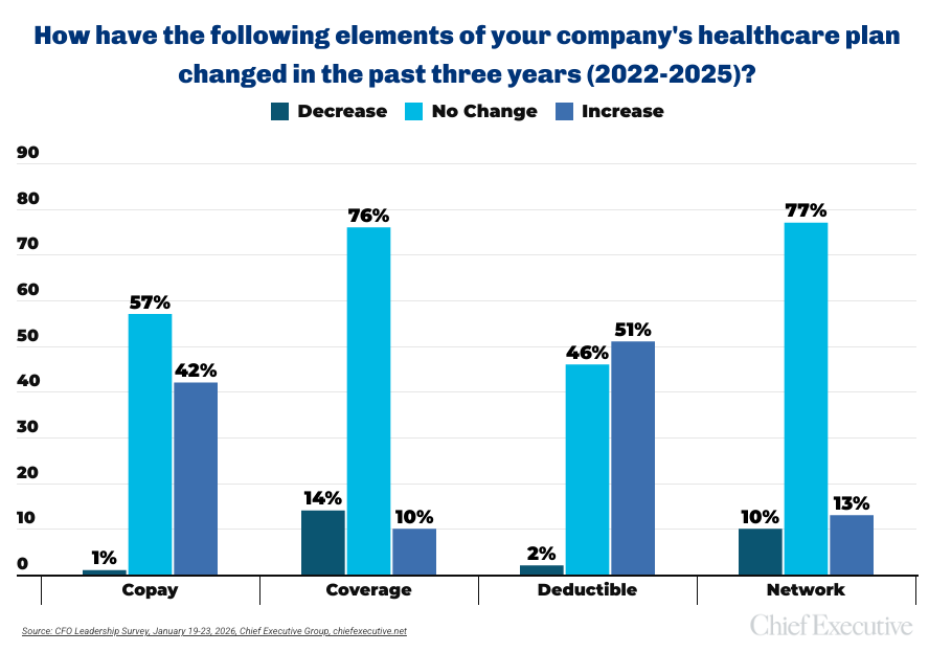
- 76 percent say coverage remains the same despite higher premiums.
- 14 percent say coverage has deteriorated.
- 77 percent report no improvement in provider networks.
- 57 percent say co-pays remain unchanged, while 42 percent say they have increased.
- 51 percent report higher deductibles.
The pattern points to a disconnect: Organizations are paying more, but most do not report measurable improvements in coverage breadth or benefit design. At the same time, higher employee contributions and out-of-pocket costs can reduce the practical value of wage gains.
“If you’re asking employees to pay more through higher copays and deductibles, then give them the tools to become better and smarter shoppers,” says Schroeder. “It’s their money. Let them chase quality, get better outcomes and be more cost effective.”
The Premium on Predictability
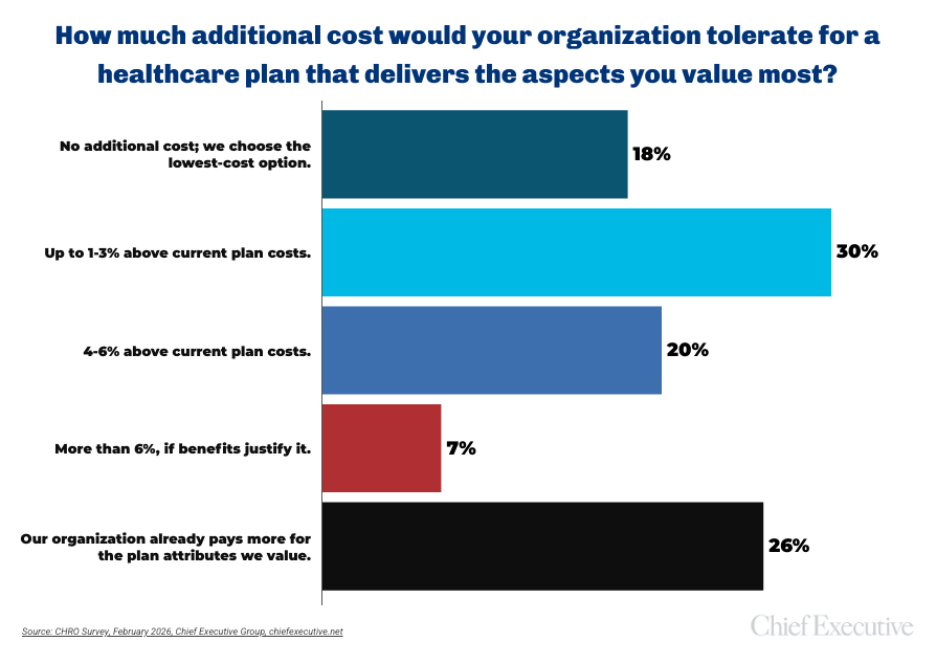
Even as costs rise, predictability appears to matter more than outright reductions.
When asked which aspects of a healthcare plan their organization values most, 67 percent of CHROs cite employee satisfaction. Predictable costs rank second, selected by 51 percent. Ease of administration follows at 41 percent, while 36 percent point to ongoing plan management by a broker or third party. Only 12 percent cite reduced regulatory or compliance risk exposure.
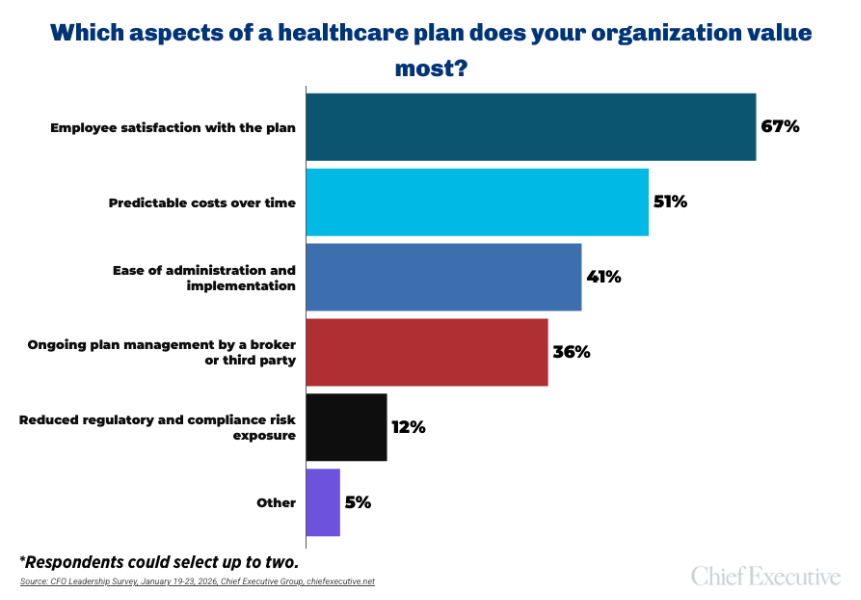
The emphasis on predictability suggests that volatility itself—not just absolute cost—is a central concern. For many employers, the inability to reliably forecast annual increases complicates budgeting, workforce planning and total compensation strategy.
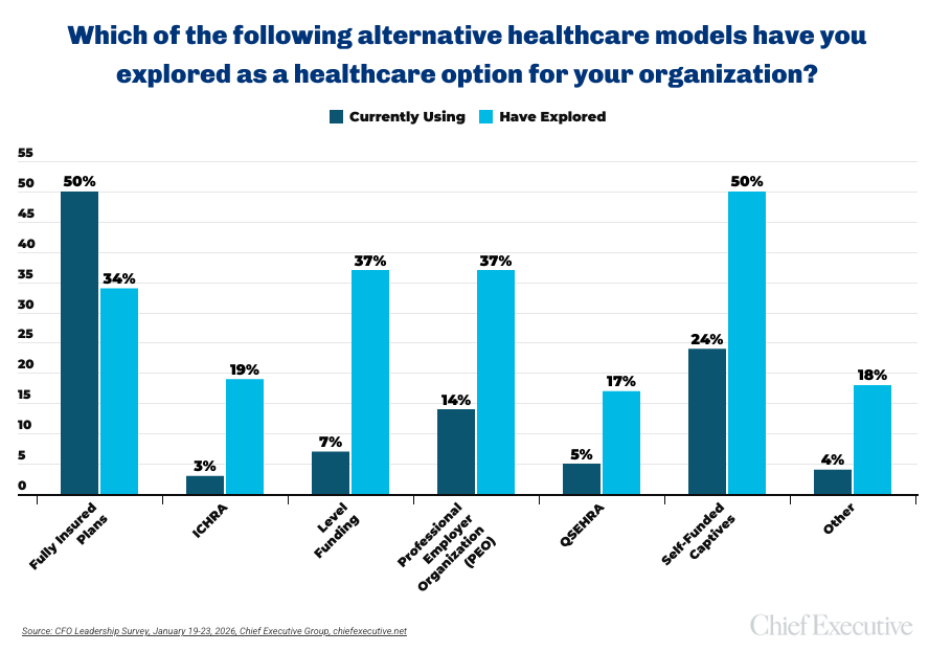
Roughly half of CFOs surveyed say they have explored self-funded captive models as an alternative solution—more than any other structure including ICHRA and QSEHRA arrangements—though whether exploration translates into adoption remains unclear.
“Five years ago, a lot of employers thought they didn’t have a choice, that they were stuck in an environment where they did not know why their costs were going up. It is getting much, much better,” Schroeder says. “There’s a long road for improvement, but we’re making good progress.”